The pupil is the black slit/circular shape in the middle of the cat’s iris (the colored part of the eye). Pupils control the amount of light entering the eye by dilating (becoming large) and constricting (becoming small/slit-like). Cats’ eyes are somewhat unique in that their pupils are vertical – so when they constrict, there is a thin vertical line. A totally dilated pupil will appear to be round.
Normal causes of dilated pupils
- Reduced light: The pupil dilates in poor light to let in more light or will constrict (shrink) in bright light to reduce the amount of light.
- Emotions: When a cat is angry or aggravated, the pupils constrict. If fearful, the eyes often dilate. When it is happy, excited or scared, they dilate.
- Pain: Cats in pain may have dilated pupils as one of the signs of discomfort.
- Certain medications: (Atropine, tropicamide, morphine, clonidine, amphetamine) and plants (such as catnip) can cause dilated pupils in cats. If your cat is on medication and has dilated pupils, contact your veterinarian who will be able to advise if this is a common side effect.
Both pupils should be equal in size, and when looked at with a bright light, they should both constrict quickly.
How do you know when dilated pupils is a serious issue?
If you suddenly notice your cats pupils look more dilated than expected, do not panic. Take them to a well lit area, or shine a light on their eyes. You should find the pupils constrict (and your cat may give you an odd look!).
However, if your cat’s pupils are not constricting regardless of what you do, or your cat has other symptoms (such as confusion or lethargy), you should seek veterinary care right away.
If concerned about your cat’s eyes, don’t hesitate to make contact with your vet.
10 Medical causes
If you notice your cat’s pupils are diluted, you’ll be wondering what’s going on. Keep in mind that cat’s pupils will naturally dilate when the lighting is low, or when they feel anxious, in pain or stressed. If the pupils remain dilate without an obvious explanation, consider there may be a medical cause:
1. Feline dysautonomia
Cats will have dilate pupils alongside a range of vague and unusual signs. Owners may simply feel their cat ‘ain’t doin’ right’. This rare disease has a poor prognosis, with less than half cats surviving past the one year mark. Those who do survive often have ongoing neurological signs.
Feline dilated pupil syndrome or Key-Gaskell syndrome
A rare condition first discovered in 1982 and caused by a dysfunction of the autonomic nervous system. This system controls parts of the body not consciously operated such as heartbeat, digestive system, and pupillary response. Young cats under three years old are most commonly affected. The cause is unknown, although some suggest that Clostridium botulinum (botulism) may be a cause.
Symptoms:
- Dilated nonresponsive pupils
- Protrusion of the third eyelid
- Loss of appetite
- Vomiting
- Straining to urinate or urinary incontinence
Treatment:
There is no cure for this condition, and the goal of treatment is to manage symptoms which may include:
- Elevated feeding position: Feed the cat in an elevated position so that gravity can help to push food down the esophagus. The cat should remain in that position for 10-15 minutes after each meal.
- Feeding tube: It may be necessary to place a feeding tube in cats who cannot eat in an upright feeding position or who are refusing food.
- Fluid therapy: To treat cats with dehydration.
- Artificial tears: To moisten and lubricate the eyes.
2. Insulinoma
The first signs of an insulinoma may be seizures and collapse, and cats are usually very unwell at diagnosis. This is another rare condition and the prognosis is poor as many have spread at time of diagnosis, and are difficult to effectively manage. As a cat is usually quite medically unstable when symptoms become obvious, owners should have them seen urgently.
A tumor of the beta cells of the pancreas that produces excessive amounts of insulin, leading to low blood sugar (hypoglycemia) which causes neurological problems and weakness.
Symptoms:
- Dilated pupils
- Increased appetite
- Weakness, especially in the hind legs
- Nausea
- Nervousness
- Rapid breathing
- Muscle twitching
- Mental confusion
- Seizures
Treatment:
If possible, surgical removal of the tumor otherwise, medical management such as steroids to promote the formation of glucose and dietary management.
3. Brain tumor
The signs of a brain tumor are hugely varied; depending on the size and exact location of the mass, as well as on whether or not it has spread. Sadly, prognosis is poor in cats, as even benign growths cause significant clinical signs, and brain tumors are very difficult and costly to treat.
Brain tumors are an abnormal growth of cells that can be benign or malignant and account for 2.2% of all tumors in cats. They can be primary, originating in the brain or its membranes, or secondary, having originated elsewhere. Approximately 70% of brain tumors are primary. There are many types of brain tumors, depending on the cells involved. The most common type of brain tumor in cats is a meningioma, a benign tumor that arises from the meninges, which is the membrane that surrounds the brain and spinal cord.
Symptoms:
Can vary on the type of brain tumor as well as its location within the brain, but may include:
- Dilated pupils
- Changes in behavior
- Seizures
- Head pressing
- Circling
- Head tilting
- Drunken gait (ataxia)
- Loss of appetite
- Disorientation
- Loss of vision
- Vomiting
Treatment:
- The treatment of choice is the surgical removal of the tumor, where possible. However, this is not possible for many brain tumors which are located deep within the brain.
- Other treatment options include radiation and or chemotherapy to shrink the tumor and slow down its progress.
- Supportive care to manage symptoms can include medications to control seizures and nausea.
4. Retinal detachment
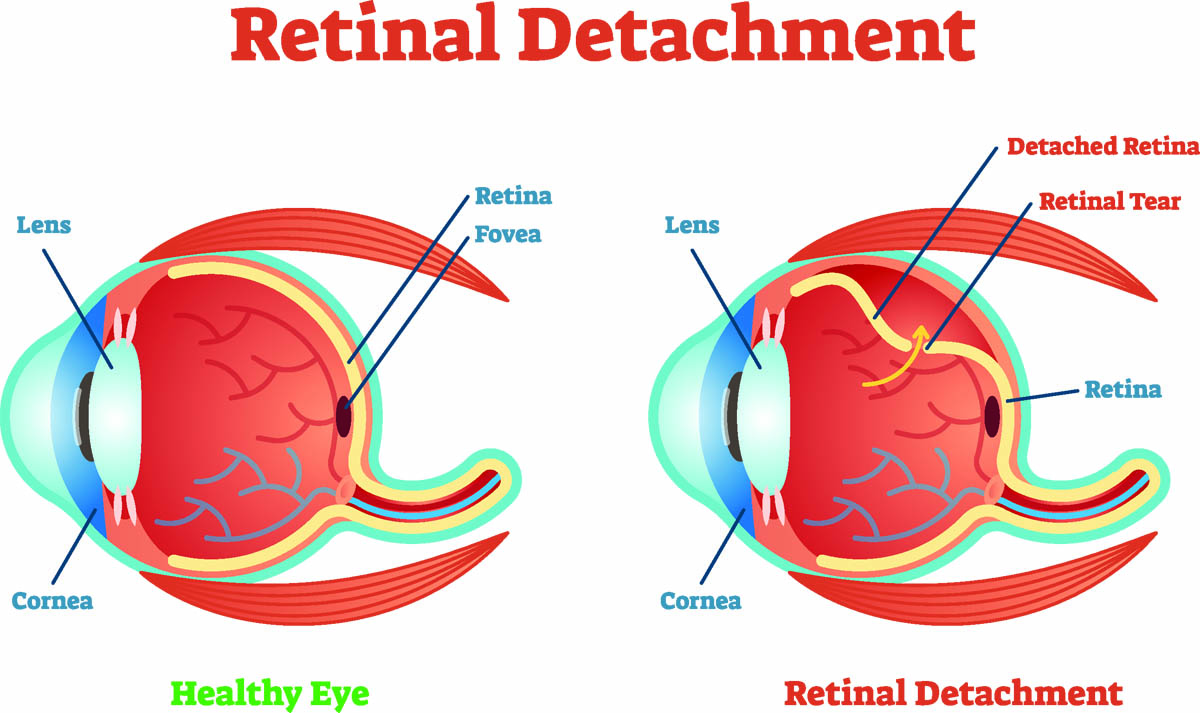
A cat who experiences retinal detachment may act confused and highly frightened. They do not understand why they suddenly cannot see, so may thrash about and bang into things around them. Prognosis is good with prompt treatment, and it is even possible for cats to recover their vision. For this reason, a cat who suddenly develops dilated pupils and blindness, needs to see their vet immediately.
Retinal detachment (RD) is a common, serious and sight-threatening disorder that occurs when the retina (a thin, transparent layer of light-sensitive tissue that lines the rear of the eye) detaches from the underlying retinal pigment epithelium layer. High blood pressure is the most common cause of retinal detachment, and hyperthyroidism (a benign tumor of the thyroid gland) is a leading cause of high blood pressure. Kidney disease leads to elevated blood pressure as the kidneys play a role in regulating blood pressure, by releasing the enzyme renin.
Other causes include trauma, infection, inflammation, cancers, glaucoma, toxins, and autoimmune disease.
Symptoms:
- Dilated pupils
- Sudden blindness
- Other symptoms will vary depending on the underlying cause
Treatment:
The goal of treatment is to address the underlying cause, which may include:
- Medication to control blood pressure.
- For those with an overactive thyroid, we’d pursue treatment options such as daily medicine, an iodine restricted diet, surgery or Radioactive iodine.
- For cats with chronic kidney disease, they are usually managed with a renal diet and other medicines, such as anti nausea medicine and phosphate binders.
5. Head trauma
A cat who suffers head trauma can present as anything from mildly dazed to comatose. The prognosis is directly dependent on the extent of the trauma, and where on the head the cat has been hit.
Any head trauma can potentially damage the brain and affect the autonomic nervous system, which as we noted above, is responsible for specific functions the cat has no direct control over such as heartbeat, digestive system, and pupillary response. A fall from a height, trauma from a car accident or an intentional hit to the head can all potentially cause injury to the brain.
Symptoms:
- Dilated pupils
- Changes in behavior
- Seizures
- Tremors
- Bleeding from the nose or ears
- Weakness
- Paralysis
Treatment:
Treatment depends on the severity of the trauma. Many cases will require hospitalization and supportive care, including fluid therapy, oxygen therapy, medications to control seizures and in some cases, surgery.
6. Glaucoma
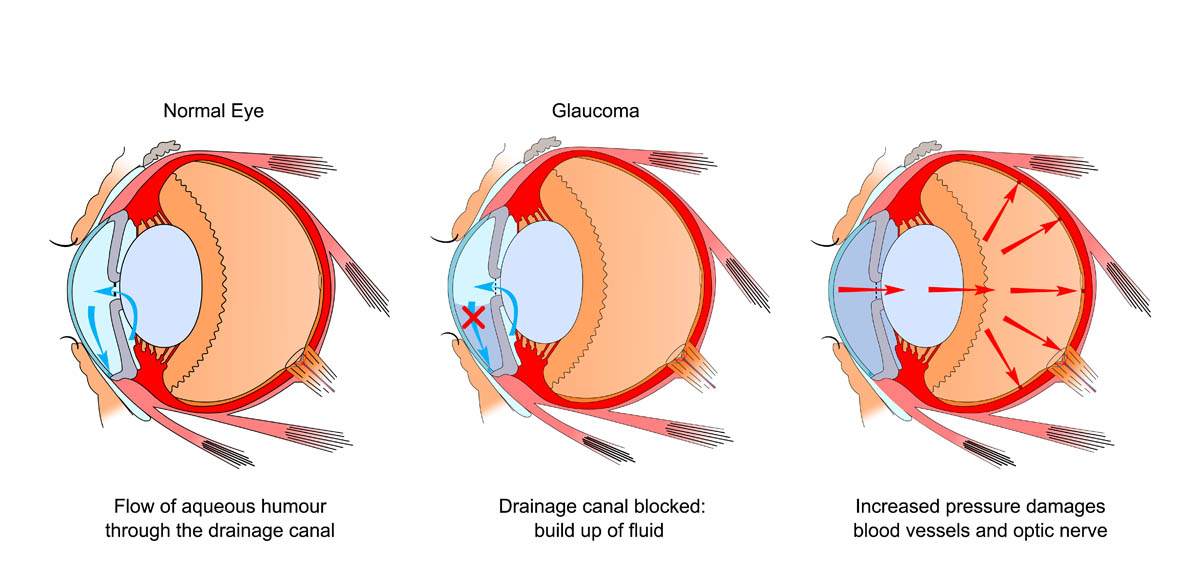
Glaucoma presents as uncomfortable and red eyes, and with time, you’ll notice your cat experiencing more pain and their eyes looking more abnormal. Only about 0.2% of cats develop glaucoma in their lifetime, making it uncommon. Prognosis depends on the underlying cause, but it is not a condition that can be reversed or cured.
An increase of pressure within the eye (intraocular pressure) can damage the optic nerve, connecting the brain to the eye. The most common cause is a blockage to the drainage system within the eye, leading to a build-up of fluid, which may be due to inflammation or infection, trauma, displacement of the lens, cataract surgery or tumours.
Symptoms:
Glaucoma is a sneaky disease and often has few signs until irreversible damage has occurred.
- Dilated pupil
- Pain
- One eye which appears larger than the other
- Squinting
- Loss of vision
Treatment:
- Medications (dorzolamide and or timolol) to bring down the intraocular pressure.
- Anti-inflammatory drugs to control inflammation.
- Painkillers to relieve pain.
- Surgical removal of the eye (enucleation) if blindness has occurred.
7. Hypocalcemia
Signs of hypocalcemia come on quickly and can be quite dramatic. Early signs include restlessness, twitching and being vocal. As this is a life-threatening condition, owners should be aware of signs and must contact their vet when symptoms first present. While generally uncommon, owners of specific cats (such as pregnant ones or those with kidney disease), should become familiar with potential symptoms.
Low level of calcium in the blood levels, impacts many systems of the body, including the heart and nervous system. There are several causes of hypocalcemia which include:
Hypoparathyroidism: Low parathyroid hormone levels in the blood, most commonly due to the accidental removal of the parathyroid gland during surgery to remove the thyroid gland in cats with hyperthyroidism. The parathyroid glands are responsible for monitoring blood calcium levels and when they decrease, secreting a parathyroid hormone to stimulate the release of calcium from the bones.
Acute or chronic kidney disease: Damage to kidneys cause a decrease in their ability to filter the blood and remove toxins (via the urine). Kidney disease affects blood calcium in two ways.
- Increased blood phosphorous pushes blood calcium into bone and other tissues.
- The kidneys are responsible for the production of vitamin D, and when levels drop, there is a decrease in gastrointestinal absorption of calcium from the food.
Milk fever: This condition occurs in female cats who are nursing kittens. Two to four weeks after queening, if the mother is not getting enough calcium in her diet and doesn’t have calcium reserves due to poor nutrition during her pregnancy, she can show signs of hypocalcemia.
Other causes of hypocalcemia include acute pancreatitis, sepsis (blood infection), ethylene glycol poisoning, hypoalbuminemia and administration of phosphate enemas.
Symptoms:
- Dilated pupils
- Changes in behaviour
- Twitching
- Stiff legged gait
- Fever
- Loss of appetite
Treatment:
The goal of treatment is to find and manage the underlying cause as well as treat symptoms of hypocalcemia.
- Slow intravenous administration of calcium gluconate 10% solution.
- Fluid therapy and nutritional support if your cat is anorexic (off their food).
- Vitamin D assists in the absorption of calcium, and therefore may also be given. Too much Vitamin D can be toxic so this should only be supplemented under veterinary guidance.
- Once the cat has stabilized, oral administration of calcium supplements are commenced. Adjustments may be necessary with both vitamin D and calcium in the first few months.
- ECG to check for cardiac abnormalities.
- Regular blood tests to monitor calcium levels to ensure they don’t become too low or too high (hypercalcemia). Monthly checks will be necessary for the first six months and then every 2-3 months after that.
8. Thiamine deficiency
Thiamine (B1) is a water-soluble vitamin that plays a vital role in many bodily functions including metabolising carbohydrates, maintaining a healthy heart and nervous system. Thiamine deficiency is rare in cats and is usually associated with those who eat a home-made diet that is either cooked in water or heat (both of which destroy thiamine) or a diet high in fish.
As it is not a common diagnosis nowadays, it may not be on your vet’s radar at first. However, treating it early on allows for full recovery. Delaying therapy can mean persistent neurological signs.
Symptoms:
- Dilated pupils
- Drooling
- Loss of appetite
- Ataxia (wobbly gait)
- Loss of righting reflexes
- Slow heartbeat
- Behaviour changes
- Twitching
- Cervical ventroflexion (necks flexed/rigid, which causes an inability to raise the head, the chin rests near the chest)
Treatment:
- Feed a nutritionally balanced diet and avoid diets containing large quantities of fish.
- Thiamine injections.
9. Venom toxicity
Venom is a form of poison secreted by several animals in defence or to kill their prey. Snakes, scorpions, spiders, and ticks are all common sources of venom toxicity in cats.
You’ll often know your cat has been bitten or stung, as you’ll see swelling or puncture marks. Signs will come on rapidly and your cat may have pain where the lesion is. Prognosis depends on the venom they’ve been exposed to; as well as the amount of venom and the location of the wound.
Symptoms:
Venom affects several body systems, including the blood, nervous system and heart and symptoms can vary depending on the type and amount of venom
- Dilated pupils
- Ataxia (wobbly gait)
- Drooling
- Confusion
- Vomiting
- Diarrhea
- Bleeding (nose, mouth, anus)
- Paralysis
- Difficulty breathing
Treatment:
Where possible, administer antivenom which counteracts the effects of the venom. Intense supportive care is essential and may include oxygen therapy, intravenous fluids, anti-nausea medication and nutritional support.
10. Anticholinergic drugs and plants
If your cat is exposed to an anticholinergic, signs come on quickly, and you’ll notice a broad range of symptoms which can include wide pupils and drooling. The prognosis will depend on what your cat has been exposed to and in what quantity. Where possible, take the offending medicine or plant with you to the vet clinic, for them to assess. The sooner your vet can start the decontamination and stabilisation process, the better for your kitty.
Drugs or plants with anticholinergic effects are substances that block acetylcholine from binding to its receptors on certain nerve cells, inhibiting parasympathetic nerve impulses. These nerve impulses are part of the autonomic nervous system responsible for several functions not consciously controlled (which includes pupil dilation and constriction). Several prescription and over the counter drugs in the following classes have anticholinergic effects, which include:
- Tricyclic antidepressants (TCA’s)
- Mydriatics/eye drops which dilate the pupils (atropine, phenylephrine, tropicamide, cyclopentolate)
- Neuroleptics/antipsychotics
- Cycloplegic drugs
- Antihistamines (Benadryl/diphenhydramine)
- Cold medications (pseudoephedrine and decongestants)
- Cardiovascular and gastrointestinal medications
- Parasympatholytic medications
Plants with anticholinergic properties include:
- Atropa belladonna (deadly nightshade)
- Brugmansia species
- Datura species
- Garrya species
- Hyoscyamus (henbane)
- Mandragora officinarum (mandrake)
- Lycopersicon (tomato)
- Solanum (nightshade)
Symptoms:
- Hyperthermia (elevated temperature)
- Drooling
- Ataxia (wobbly gait)
- Behavioural changes
- Lethargy
- Dilated pupils
- Sensitivity to bright light
- Gastrointestinal upset
- Delayed gastrointestinal emptying (decreased bowel motions)
- Urinary retention
- Seizures
- Decreased heart rate
Treatment:
Gastrointestinal decontamination is recommended if ingestion is recent, followed by activated charcoal to bind to any remaining toxins in the gastrointestinal tract.
The antidote for anticholinergic toxicity is Physostigmine, which works by increasing extracellular levels of the neurotransmitter acetylcholine, which counteracts the effects of the anticholinergics.
Supportive care may include intravenous fluids to correct pH disturbances or electrolyte imbalances, oxygen therapy, pilocarpine to reduce pupil dilation, diazepam to control seizures.
Diagnosis
Your veterinarian will perform a complete physical examination and may need to perform some diagnostic tests to determine the cause.
He will carefully examine the eyes and obtain a medical history from you.
- How long have symptoms been present?
- Have you noticed any other symptoms?
- Is the cat’s vision affected?
- Is the cat on any medication?
- Does the cat have any underlying medical conditions?
- Is there any chance of toxicity?
Diagnostic workup:
- Baseline tests – Biochemical profile, complete blood count, and urinalysis to check the overall health of your cat and evaluate for diabetes (glucose in the blood and urine) and other underlying diseases
- Blood pressure measurement – This test uses a cuff and doppler to measure the pressure within the arteries to check for abnormal blood pressure.
- Ultrasound – To evaluate the eyes and organs such as the pancreas, for signs of inflammation, infection or tumours.
- CT scan – An advanced non-invasive medical imaging technique that uses a combination of x-ray imaging and a digital computer to produce detailed 3-dimensional images to evaluate for brain tumours.
- Tonometry – A tonometer is an ophthalmic device with a probe that is used to measure the pressure inside the eye (intraocular pressure) to evaluate for glaucoma. Anaesthetic eye drops are applied to the eyes and the tonometer is placed onto the cornea to gauge IOP.
- Ophthalmoscopy – An examination of the back part of the cat’s eye using an ophthalmoscope to evaluate the retina, optic nerve and blood vessels.
- Gonioscopy – A gonioscope is used in conjunction with a slit lamp to evaluate the internal drainage system of the eye (anterior chamber) where the cornea and iris meet.
What if my cat has dilated pupils and appears disoriented?
Many of the causes of dilated pupils listed above show symptoms of both dilated pupils and unusual or disoriented behavior. It is important to try to determine the exact cause (such as a plant toxin or abnormal salt levels) so that treatment can be directed to the cause. Your cat may move cautiously especially in bright light due to abnormal vision – think of how you squint and wear sunglasses after a visit to the ophthalmologist when your eyes are dilated.
Some of the causes of pupil dilation can also cause acute blindness (which may be irreversible). Your cat may be reacting strangely to the sudden, complete loss of vision.
Any cat showing dilated, non-responsive pupils and unusual behavior should be examined at the veterinary clinic as soon as possible. The same is true for cats with anisocoria – pupils of different sizes.
What should you do?
If you notice your cat has dilated pupils, move him to a source of light, or shine a flashlight or penlight in the eyes to see if they constrict (go smaller). If there is no change, despite exposure to light, consult your veterinarian. If your cat is stressed or has just woken up, it may take a moment or so for her pupils to return to normal size. Once settled, recheck her pupils with a light.
If your cat shows dilated pupils and is behaving strangely (such as having trouble walking through the house), she should be seen by a veterinarian ASAP as she may be experiencing sudden blindness.


