What is liver disease?
Also known as hepatic disease, liver disease is a collection of diseases, all of which result in damage to the liver leading to impaired function. Liver disease can be acute (sudden onset) or chronic (slow and progressive). Cats of any age can develop liver disease, however, portosystemic shunt or toxic hepatopathy (ingestion of toxins or drugs) are more common in younger cats while primary cancers typically occur in cats who are ten years or older.
The liver is the largest internal organ of the body, and it is responsible for several metabolic, functional and detoxification processes. It is located in the abdomen, under the diaphragm. The liver is the only organ in the body that is capable of regenerating itself and has an amazing functional reserve with up to 70% of the functional mass impaired before symptoms may present. Two blood vessels enter the liver, the hepatic portal vein contains deoxygenated blood from the spleen, pancreas, and digestive system and the hepatic artery contains oxygen-rich blood from the lungs.
Functions performed by the liver
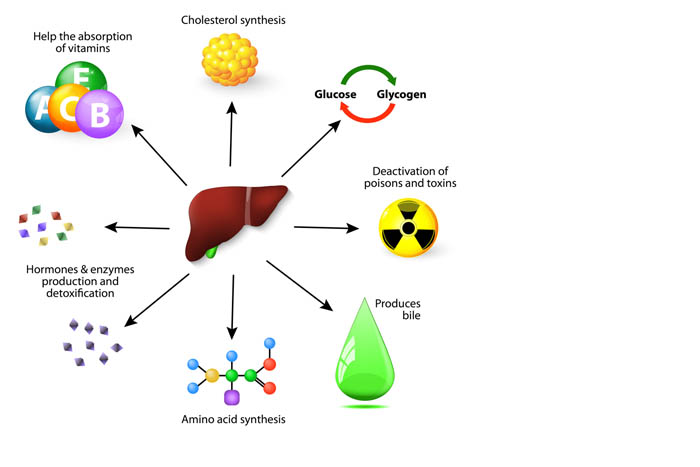
The cat’s liver performs multiple critical functions, which includes:
- Metabolises drugs and medications.
- Processes nutrients from the blood and removes waste products.
- Produces and secretes bile, which aids digestion and absorption of fats. Bile is a greenish-yellow fluid that consists of bile acids and waste products such as bilirubin.
- Breaks down hemoglobin to create metabolites that are added to bile as a pigment (bilirubin).
- Produces specific enzymes which aid the digestion of food.
- Converts most sugars into glycerine which it stores up as glycogen until required.
- Stores fat-soluble vitamins A, D, E and K which need bile to be absorbed by the body. The liver also stores iron, copper, and zinc.
- Production of all blood clotting factors with the help of vitamin K.
- Manufacture of certain hormones such as insulin-like growth factor 1 (IGF-1) which stimulates growth, angiotensinogen regulates blood pressure and thrombopoietin, which regulates the production of platelets.
- Regulating chemicals in the blood.
- Balances the hormones estrogen and testosterone.
- Produces certain proteins for blood plasma, including albumin, fibronectin, and globulins.
- Processes hemoglobin for its iron content.
- Changes ammonia, a toxic by-product of protein metabolism into urea, which is excreted in the urine.
Causes
Hepatic lipidosis
(Idiopathic hepatic lipidosis or fatty liver disease)
Hepatic Lipidosis is the most common type of liver disease in the cat and occurs when your cat becomes anorexic (stops or reduces the amount of food he is eating), the body begins to use fat stores as fuel which the liver breaks down. Unfortunately, the liver sometimes becomes overwhelmed and is unable to process this fat as quickly as necessary, leading to a build-up of fat in the liver, which interferes with normal liver function.
Cholangitis
(Inflammatory liver disease)
The second most common form of liver disease, that is caused by several related inflammatory and or infectious disorders of the liver and/or the biliary tract. Cholangitis relates to infection or inflammation of the bile duct, and cholangiohepatitis is inflammation of the biliary system and by extension, the liver. Causes of infection may often include FIP, Pancreatitis, inflammatory bowel disease (IBD), bacterial infection, parasitic infection (including toxoplasmosis).
Damage by toxins
(Toxic hepatopathy)
As the liver is responsible for processing toxins from household cleaners, insecticides, plants, drugs and other toxins, it is vulnerable to damage when the cat consumes or is exposed to toxic substances (hepatotoxins). There are too many possible toxins to list in this article, but some common ones include excess amounts of vitamin A and iron, Naphthalene (found in mothballs), Methimazole, Xylitol, Diazepam, Effexor, acetaminophen and aspirin.
Toxoplasmosis
Caused by intracellular protozoa known as Toxoplasma gondii, most infected cats will show no symptoms of infection, however in some cases damage to various organs can occur, including the liver. This is most often in immunocompromised cats such as those with FIV.
Tumours
There are many different types of tumours that affect the liver. Primary liver cancer (originating in the liver) is uncommon in cats, hepatocellular carcinoma and bile duct tumours are the most common. Primary liver tumours make up only 1-3% of cancers in cats. Most malignant tumours of the liver are secondary, having originated from another site and spread to the liver. Benign tumours are far more common in cats.
Portosystemic shunt
Portosystemic shunts are abnormal communications between the portal and systemic venous system which allows intestinal blood to be delivered to the systemic circulation before hepatic detoxification. A shunt means that blood bypasses the liver, resulting in blood not being detoxified by the liver and a rise in toxins. Portosystemic shunts may be congenital or acquired, most shunts in cats are congenital (known as CPSS), and cats demonstrate clinical signs within 12 months of age.
Clinical signs
- Loss of appetite
- Weight loss
- Drooling, due to nausea
- Lethargy
- Diarrhea
- Vomiting
- Jaundice (icterus): Signs of jaundice are yellowing of the eyes, skin and mucous membranes, due to hyperbilirubinemia, high levels of bilirubin in the blood
- Ascites (abdominal effusion): Build-up of fluid in the peritoneal cavity caused by portal hypertension (high blood pressure) in the portal vein of the liver
- Polyuria (increased urination)/polydipsia (increased thirst)
- Hepatomegaly (enlargement of the liver) or microhepatica (small liver)
- Dark coloured but clear urine caused by the presence of bilirubin
- Bad breath
- Melena (dark tarry stools) due to the liver losing its ability to produce clotting factors resulting in internal bleeding
- Hepatic encephalopathy (decline in brain function) due to a build-up of toxins in the bloodstream which cross the blood-brain barrier
- Coma
Diagnosis
The veterinarian will perform a physical examination of your cat and obtain a medical history from you, including any current medical conditions he may have, medications he’s on and exposure to toxins.
Diagnostic workup:
- Complete blood count: May reveal the presence of poikilocytes, which are abnormally shaped red blood cells. Anemia may also be present. Reduced white blood cells or platelets may indicate portal hypertension.
- Urinalysis: To look for ammonium biurite crystals if your cat has a portosystemic shunt and/or bilirubin in the urine.
- ALT and AST tests: Changes to the liver enzymes ALT (alanine aminotransferase) and AST (aspartate aminotransferase). The ALT test determines the level of this enzyme in the blood, which increases when damage to the liver cells has occurred. AST is an enzyme in skeletal and cardiac muscle cells, the brain and red blood cells. Elevated AST in the blood is also an indicator of liver disease, although as it is found in other organs, it is not as specific for liver cell injury as elevations in ALT.
- Bilirubin: This is a major breakdown product of red blood cells. When red blood cells wear out, they are trapped in the spleen and destroyed, releasing bilirubin into the blood. This type of bilirubin is called unconjugated. This bilirubin is transported in the blood to the liver, where it is taken up and conjugated (joined with glucuronic acid). This conjugated form may either be stored in the liver cells or excreted into the bile. Bilirubin levels are increased in cats with liver disease, gallbladder disease or have excessive destruction of red blood cells (known as hemolysis).
- Blood urea nitrogen: Low blood urea nitrogen (BUN), albumin, glucose, cholesterol reflect the liver’s inability to metabolise urea and glucose or produce albumin or cholesterol.
- Bile acids tolerance test: This involves taking a blood sample from your cat and then feeding him a fatty meal, followed by a second blood test two hours later. When a cat eats, bile is released into the small intestine to assist with the digestion of fats (lipids). The bile is then absorbed by the intestine and returned to the liver where it is removed from the bloodstream. In a cat with liver disease, this process doesn’t occur as efficiently, and levels of bile remain high in the blood.
- Ultrasound: An ultrasound can give your veterinarian an idea of the size and shape of your cat’s liver and gallbladder, to detect gallstones and biliary obstruction (blockage of the flow of bile from the liver), and evaluate the blood vessels. Intrahepatic (inside the liver) are easier to see on ultrasound than extrahepatic (outside the liver) vessels.
- X-Ray and/or ultrasound: An x-ray may be taken to give your veterinarian an idea of the size and shape of your cat’s liver. An X-ray may also detect the presence of tumours and blockages in the bile duct.
- Biopsy: A liver biopsy is taken to determine the exact type of liver disease, may occur at the same time as the ultrasound.
- Serologic Testing: Testing for diseases such as FeLV, FIV, FIP, and toxoplasmosis may be taken as these diseases are associated with some liver disorders in cats.
- Coagulation tests: A series of blood test to measure the body’s ability to form a blood clot. Typical tests include aPTT, INR, fibrinogen and platelets.
Treatment
Hepatic lipidosis
- Intensive nutritional support. Most frequently, this involves feeding a calorie-dense, high protein food via a feeding tube either directly into the stomach or esophagus.
- Appetite stimulants for cats who are well enough to eat by themselves but anorexic.
Cholangitis/cholangiohepatitis complex
- Antibiotics to treat bacterial infections.
- Immunosuppressive drugs such as corticosteroids to reduce inflammation.
Damage by toxins
- Aggressive decontamination is required to treat toxicity in cats. This includes the removal of toxins from the body such as inducing vomiting or gastric lavage (stomach pumping) or activated charcoal to prevent further absorption.
Tumours
If possible, surgical removal of malignant and benign tumours. Primary liver tumours don’t respond well to chemotherapy
Portosystemic shunt
- Surgical ligation if physically and financially possible.
- A low-protein prescription diet.
Supportive care
- Anti-nausea medications: To control nausea and vomiting.
- Fluid therapy: To correct dehydration and electrolyte imbalances.
- Antibiotics: To treat any underlying bacterial infection.
- Vitamin K: This fat-soluble vitamin is necessary for the formation of certain clotting factors, as the liver fails, clotting factors decrease, which can lead to coagulopathy (blood clotting disorders). Administration of Vitamin K may help to restore normal blood clotting.
- Plasma transfusion: If blood clotting disorders develop.
Prevention
Hepatic lipidosis is often caused by a cat’s refusal to eat; obesity also predisposes a cat to this disease. When changing your cat’s diet, do so slowly by mixing a small amount of the new food in with the old. Gradually increase the new food while decreasing the old food over 5-7 days. Closely watch your cat for signs of appetite loss during this time.
Only administer medications prescribed by a veterinarian and always monitor for side effects.
Keep all medications, household cleaners, and other toxins away from your cat in a locked cupboard. I also recommend using natural products such as white vinegar when cleaning as much as possible — the fewer chemicals in the home the better for all of us.
Be diligent when it comes to plants and cut flowers in your home. Many are highly toxic to cats; some cause liver damage; others cause kidney damage. Regardless of the organ(s) affected, pet owners, need to be diligent when it comes to plants and flowers.

